A Different Kind of Match: SHSU-COM Student Doctor Becomes Stem Cell Donor
A Different Kind of Match: SHSU-COM Student Doctor Becomes Stem Cell Donor
As fourth-year medical students prepare for Match Day, one SHSU-COM student doctor reflects on a different kind of match after becoming a life-saving stem cell donor.
Each March, soon-to-be doctors across the country wait to learn where they will train next on Match Day. For patients facing certain blood cancers and serious blood disorders, however, a different kind of match can mean the difference between life and death. Stem cell transplants depend on finding a donor whose immune system closely matches their own, a search that can take weeks, months or even longer.
Earlier this year, Sam Houston State University College of Osteopathic Medicine (SHSU-COM) student doctor Uttam Gyawali became that match for someone in need.
Gyawali, who grew up in the Houston area, is one of eight siblings and was raised in an immigrant family that emphasized caring for others and sharing what they had. He joined the National Marrow Donor Program (NMDP) registry almost by chance.

While helping organize a meeting through the Asian Cancer Council, a coalition focused on cancer awareness and outreach, a representative spoke about the national donor registry and invited attendees to complete a simple cheek swab. During the presentation, the speaker explained that expanding representation in the registry is essential so patients with a wide range of genetic markers have the best chance of finding a compatible stem cell donor. Gyawali decided to sign up that day, adding his name to a national database of potential donors who could one day be called upon to help a patient in need of a stem cell transplant.
The NMDP registry connects volunteer donors with patients whose doctors are searching for a compatible match. Stem cell transplants rely on matching immune system markers called HLA markers, which are inherited. Because of this, patients are most likely to match with donors whose genetic markers are similar to their own. A strong registry includes a wide range of genetic markers, so patients have the best possible chance of finding a life-saving donor.
When certain genetic profiles are missing or limited in the database, patients who share those markers can face longer searches for a compatible donor. Expanding the registry helps ensure that more genetic markers are represented, improving the likelihood that every patient can find a match when they need one most.
More than a year after joining the registry, Gyawali received the call that his genetic markers were a match for a patient in need.
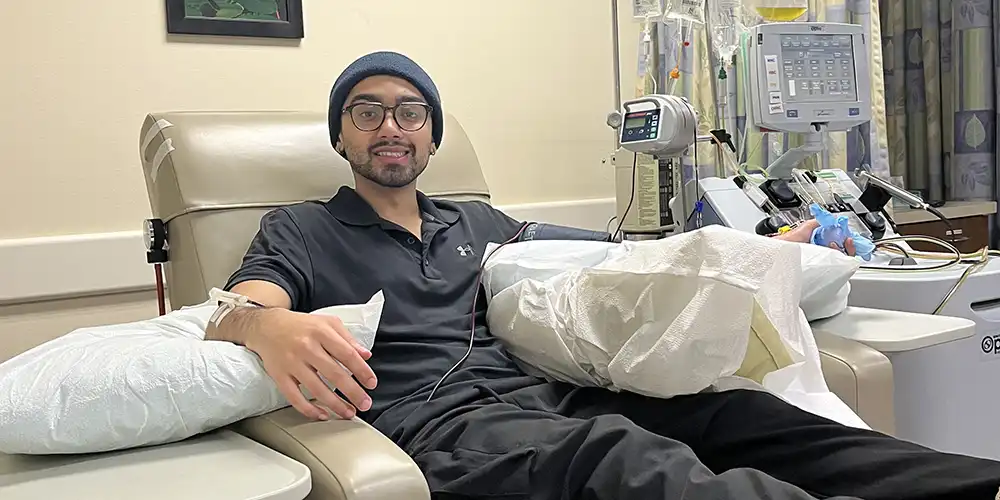
After several rounds of testing confirmed the match, he traveled to Dallas in January to donate peripheral blood stem cells, the most common form of donation. In the days leading up to the procedure, donors receive medication that encourages the body to produce more stem cells in the bloodstream. Those cells are then collected through a process similar to donating blood.
For Gyawali, the procedure itself was surprisingly straightforward. Donors remain awake throughout the process, which typically takes several hours, and most return to normal routines shortly afterward.
The timing of the call carried personal meaning. Gyawali learned he had been selected as a donor just one day after the passing of his father.
Growing up, Gyawali saw firsthand how chronic health conditions can affect a family, particularly through his father’s experiences navigating the healthcare system. Those moments helped shape his decision to pursue medicine and the kind of physician he hopes to become.
Even while processing the loss of his father, Gyawali never questioned whether he would move forward with the donation.
“This was what I signed up for,” he said. “If someone needs help and you have the ability to give it, then you should.”
That sense of service is something he traces back to his upbringing. Several members of his family have pursued careers in healthcare. One sister is a pediatrician, another is completing residency training in psychiatry, and his twin brother is also attending medical school.
“My parents always encouraged us to care for other people and share what we have,” he said. “Helping someone else like this just feels natural.”
While Gyawali knows only limited information about the patient who received the transplant, he often finds himself wondering how the treatment is progressing. Registry guidelines allow donors and recipients to exchange information after a waiting period, depending on program policies.
For Gyawali, the experience reinforced how a small decision can carry enormous impact. Joining the NMDP registry begins with a simple cheek swab used to identify a volunteer’s HLA markers. If a match is found, donors may be called upon to provide stem cells through a process similar to donating blood.
What began with a simple cheek swab became a potentially life-saving match.
This page is maintained by :
-
SHSU-COM Director of Marketing, PR & Communications: Brittany Foreman